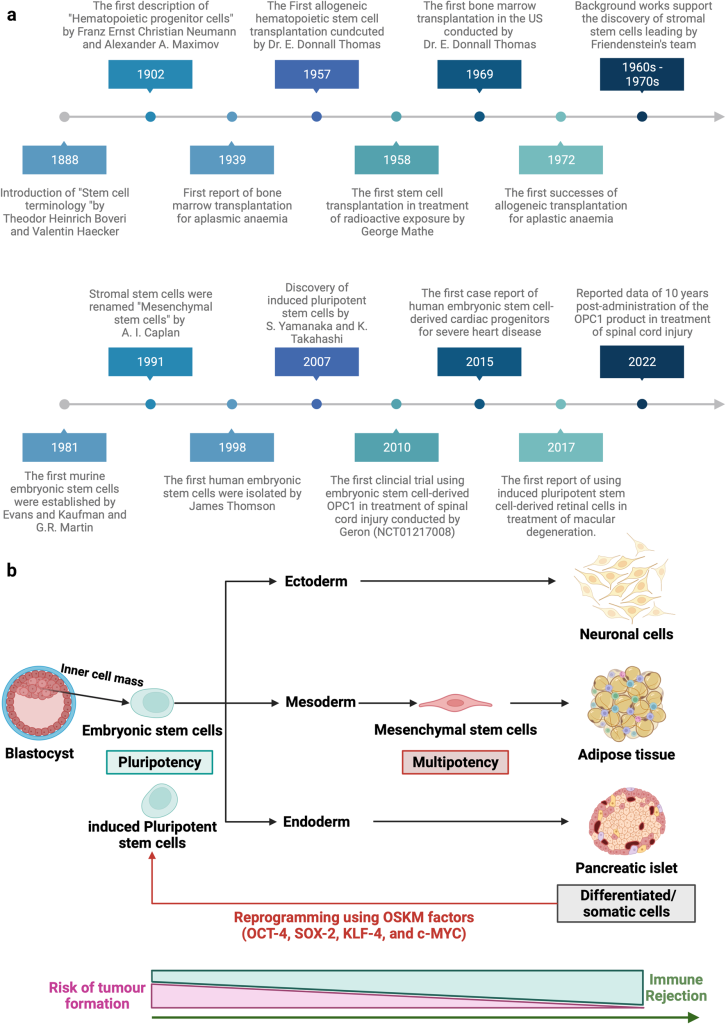
Regenerative medicine and cellular therapies represent a massive paradigm shift in how modern healthcare approaches deeply complex diseases. At the forefront of this medical frontier is stem cell therapy, an advanced intervention that relies on replacing or repairing diseased tissues with healthy, functional progenitor cells. Leading healthcare institutions such as Liv Hospital emphasize that the success of these profound treatments is not merely rooted in the transplant procedure itself. Instead, the foundation of a successful outcome is entirely dependent on the meticulous preliminary stages. A rigorous approach to diagnosis and evaluation forms the absolute bedrock of patient safety and therapeutic efficacy, ensuring that every medical intervention is precisely tailored to the individual’s unique biological and genetic landscape.
The Foundation of Pre-Transplant Assessment
The process of preparing a patient for advanced cellular therapy is highly intricate and demands an exact scientific approach. Before any therapeutic action can commence, a multidisciplinary team composed of oncologists, hematologists, specialized transplant physicians, and pathologists must conduct a thorough medical investigation. The primary objective is to ascertain the precise nature of the underlying disease, completely evaluate the systemic health of the patient, and determine the optimal source for the cellular graft.
This phase requires mapping out the genetic, molecular, and physiological profile of the disease. Medical professionals cannot simply administer cellular therapies uniformly; the protocols must be dictated by the specific trajectory of the patient’s condition. This intensive mapping prevents the implementation of ineffective treatments and mitigates severe risks associated with immunological rejection or procedural toxicity.
Key Methodologies in Cellular Diagnostics
Medical professionals utilize a vast battery of highly sophisticated laboratory and imaging tests to achieve a complete medical picture. The cornerstone of this diagnostic phase involves bone marrow aspiration and biopsy. During this procedure, physicians extract a small sample of the spongy tissue and fluid from inside the pelvic bone to microscopically examine the cellular composition. This allows pathologists to see exactly how the marrow is functioning and to identify any malignant cells hiding within the cavity.
Flow cytometry is then frequently employed to analyze the physical and chemical characteristics of the cells within the extracted sample. This technology uses lasers to count and sort cells, identifying abnormal malignant populations with remarkable accuracy based on specific markers on the cell surface. Additionally, Human Leukocyte Antigen (HLA) typing is a mandatory, high-resolution genetic test used when matching patients with potential donors. This specific immunogenetic matching process is vital to minimize the risk of Graft-Versus-Host Disease (GVHD), a severe and potentially fatal complication where the newly transplanted immune system recognizes the recipient’s body as foreign and attacks it.
Precision in Hematological Malignancies
The necessity for absolute exactitude becomes particularly evident when medical teams are managing severe hematological malignancies. For instance, highly detailedStem Cell Diagnosis and Evaluation protocols are strictly enforced for patients battling various forms of lymphatic cancer. In these high-stakes scenarios, the evaluation process determines the exact microscopic subtype and systemic stage of the lymphoma, meticulously measuring how deeply the disease has infiltrated the bone marrow, lymph nodes, or other major organs.
This precise diagnostic clarity enables the medical board to make a critical decision: whether an autologous transplant (harvesting and utilizing the patient’s own clean cells) or an allogeneic transplant (utilizing perfectly matched cells from a healthy donor) presents the highest probability of a durable, long-term remission. Without this targeted evaluation, choosing the correct pathway would be impossible.
Rigorous Evaluation of Physiological Resilience
Beyond analyzing the disease itself, physicians must rigorously evaluate the physical resilience and overall fortitude of the patient. Stem cell transplantation is an aggressive, systemic medical procedure that places immense physiological stress on the human body, particularly during the initial conditioning phase, which often involves high-dose, ablative chemotherapy or total body irradiation.
Extensive organ function testing is therefore a non-negotiable prerequisite. This typically includes detailed echocardiograms to assess cardiac ejection fraction and muscle strength, advanced pulmonary function tests to measure lung capacity and oxygen exchange rates, and comprehensive blood panels to verify optimal liver and kidney function. Furthermore, meticulous infectious disease screening is conducted to identify any dormant viruses, such as Cytomegalovirus (CMV) or Hepatitis, which could dangerously reactivate once the patient’s immune system is purposefully suppressed to accommodate the new graft.
The continuous evolution of diagnostic technologies ensures that pre-transplant evaluations are becoming increasingly precise with each passing year. Modern innovations in next-generation sequencing and molecular diagnostics currently allow medical teams to detect minimal residual disease—microscopic levels of cancer that were completely invisible to older technologies. This leads to far more accurate prognostic assessments and customized timelines for interventions. By prioritizing exact cellular mapping, rigorous physiological assessments, and collaborative review, the medical community continues to elevate the safety standards and long-term survival rates associated with these powerful regenerative therapies, offering highly targeted pathways for patients facing formidable health challenges.